Table of Contents
Toggle- Is it Dry Skin or Athlete’s Foot? Understanding Dry Skin
- Is It Dry Skin or Athlete’s Foot? Understanding Athlete’s Foot
- Distinguishing Dry Skin from Athlete’s Foot: Key Differences
- Avoiding Missteps: The Significance of Professional Diagnosis
- Home Remedies and Self-Care for Dry Skin
- Treatment Options for Athlete’s Foot
- Conclusion
Distinguishing between dry skin and an athlete’s foot is crucial for implementing appropriate treatment and preventing complications. Mistaking one for the other can lead to ineffective treatment, prolonged discomfort, and the potential spread of infection.
Dry skin is a common condition, affecting millions of people worldwide. It can occur at any age and is often exacerbated by environmental factors like low humidity and harsh soaps. Athlete’s foot, a fungal infection, is also prevalent, affecting approximately 15–25% of the global population.
This article will delve into the key differences between dry skin and athlete’s foot, guiding you through their causes, symptoms, and treatment options. By understanding these distinctions, you can effectively manage your foot health and seek appropriate medical attention when necessary.
Is it Dry Skin or Athlete’s Foot? Understanding Dry Skin
This section investigates the details of dry skin, a common condition affecting individuals of all ages. It explores the causes, symptoms, and risk factors associated with dry skin, particularly as it pertains to the feet.
i. Definition and Causes of Dry Skin
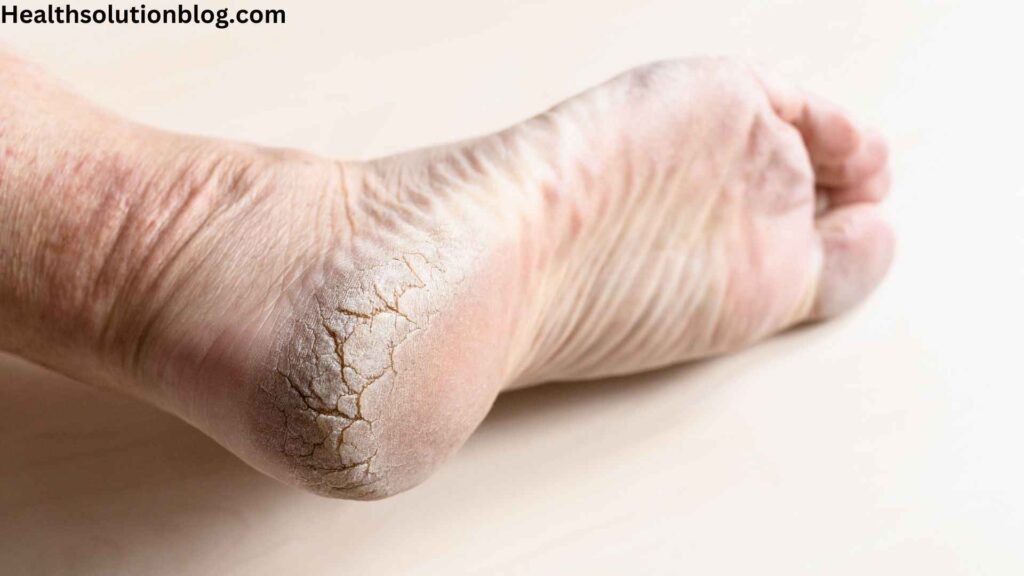
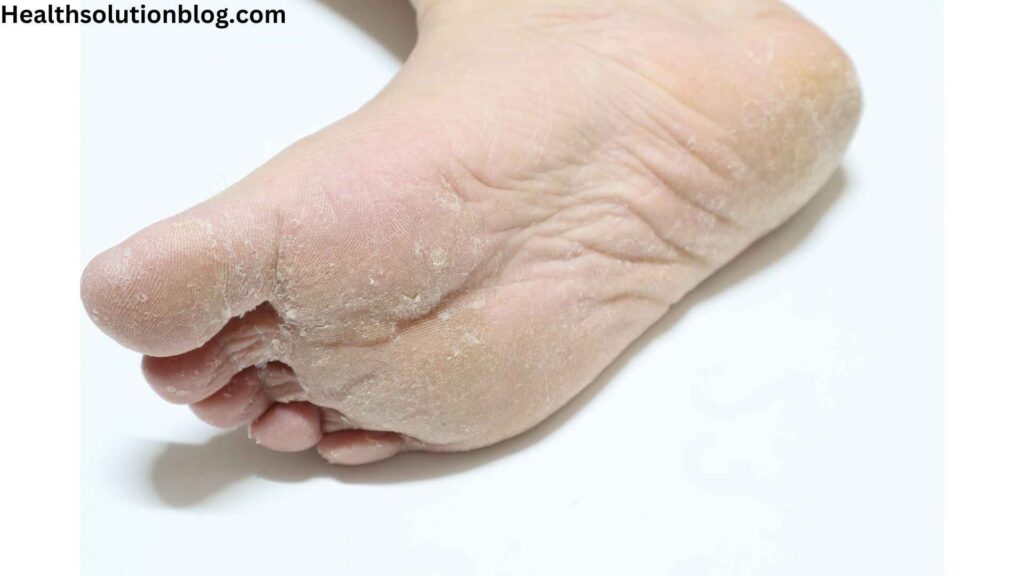
Dry skin, also known as xerosis, is a common condition characterized by a lack of moisture in the outermost layer of the skin. This moisture deficiency can be caused by various factors, including:
- Environmental factors: Low humidity, harsh soaps, and frequent exposure to hot water can strip the skin of its natural oils, leading to dryness.
- Medical conditions: Certain medical conditions, such as eczema, psoriasis, and diabetes, can increase the risk of dry skin.
- Aging: As we age, our skin naturally produces less oil, making it more prone to dryness.
ii. Common Symptoms and Characteristics
Dry skin typically manifests as:
- Rough, flaky skin
- Skin tightness and discomfort
- Itching, which can be mild or severe
- Cracks or fissures in the skin
These symptoms can appear in any part of the body, including the feet.
iii. Risk Factors that Contribute to Dry Skin
Several factors can increase the likelihood of developing dry skin:
- Genetic predisposition: Some individuals are genetically predisposed to dry skin due to variations in skin barrier function.
- Occupational exposure: Individuals working in environments with low humidity or frequent exposure to chemicals are more susceptible to dry skin.
- Lifestyle habits: Frequent bathing, using harsh soaps, and not moisturizing regularly can exacerbate dry skin.
iv. Impact on Skin Health and Comfort
Dry skin can significantly impact skin health and comfort. It can lead to:
- Impaired skin barrier function: Dry skin is more susceptible to irritation, infections, and allergens.
- Reduced skin elasticity: Dry skin can become less elastic, making it more prone to cracking and tearing.
- Discomfort and itching: Dry skin can cause significant discomfort and itching, affecting daily activities and sleep quality.
Proper skin care and moisturizing are essential for managing dry skin and maintaining overall skin health.
Is It Dry Skin or Athlete’s Foot? Understanding Athlete’s Foot
i. Definition and Causes of Athlete’s Foot
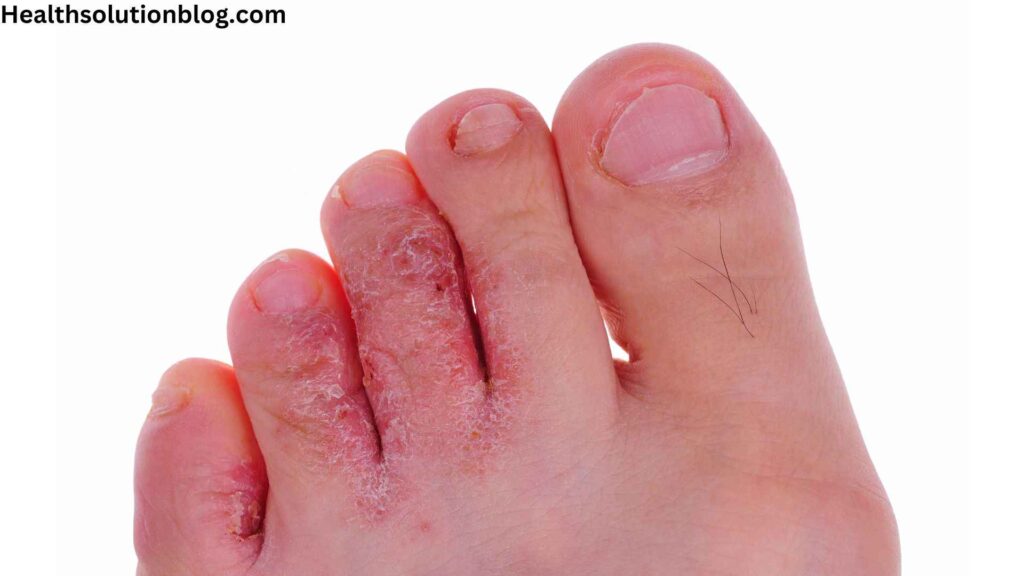
Athlete’s foot, medically known as tinea pedis, is a fungal infection that affects the skin of the feet. It is caused by a group of fungi called dermatophytes, which thrive in warm, moist environments. These fungi invade the outermost layer of the skin, causing a range of uncomfortable symptoms.
ii. Common Symptoms and Signs
Athlete’s foot typically presents with the following symptoms:
- Intense itching and burning sensation between the toes
- Red, scaly rash, often starting between the toes
- Peeling or flaking skin on the soles of the feet
- Blisters or small ulcers on the feet
- Cracking or fissuring of the skin
In severe cases, an athlete’s foot can spread to the toenails, causing thickening, discoloration, and crumbling of the nail.
iii. How It Spreads and Who Is at Risk
Athlete’s foot is highly contagious and can spread through direct contact with an infected person or contaminated surfaces, such as shower floors, locker room benches, or shared towels. Individuals at increased risk include:
- Athletes, particularly those who engage in activities that cause sweaty feet
- People who wear tight-fitting or non-breathable footwear
- Individuals who frequently use public showers or locker rooms
- Those with weakened immune systems
iv. The Importance of Prompt Diagnosis and Treatment
Prompt diagnosis and treatment of athlete’s foot are crucial to prevent the infection from spreading to other areas of the body or other people. Untreated athlete’s foot can also lead to secondary bacterial infections, causing further complications.
Distinguishing Dry Skin from Athlete’s Foot: Key Differences
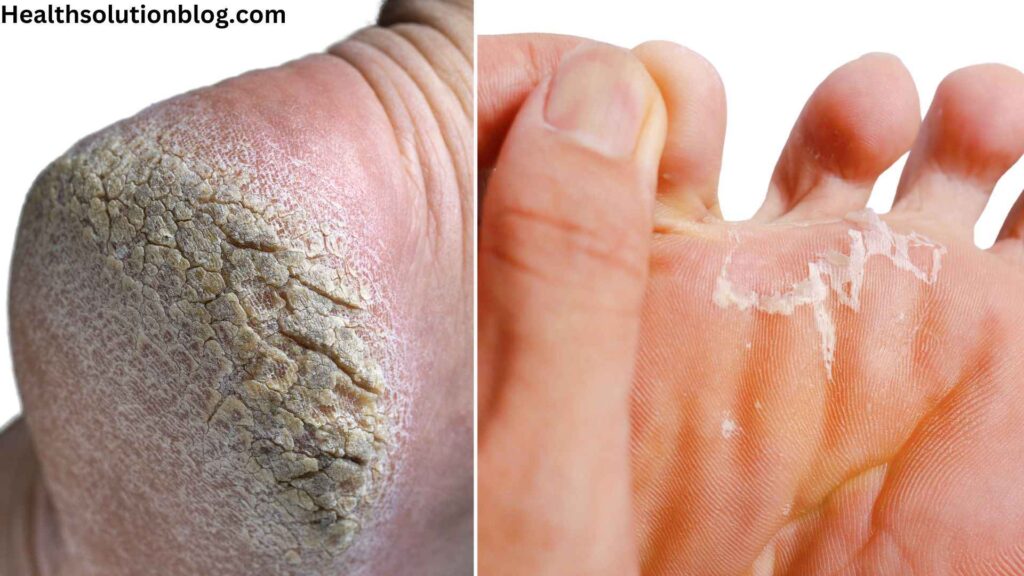
Dry skin and athlete’s foot may share some overlapping symptoms, but understanding their key distinctions can guide you toward a proper diagnosis and treatment. This section delves into the critical differences between these two conditions, empowering you to make informed decisions about your foot health.
i. Skin Appearance and Texture
Dry Skin: Dry skin typically appears rough, flaky, and sometimes scaly. It may feel tight and uncomfortable, especially after bathing or exposure to dry air.
Athlete’s Foot: Athlete’s foot often presents with a red, scaly rash, typically starting between the toes. The skin may also peel or flake, and in severe cases, blisters or ulcers may develop.
ii. Itching and Discomfort
Dry Skin: Dry skin can cause mild to severe itching, which can worsen at night or after bathing. The discomfort is generally localized to the affected area.
Athlete’s Foot: Athlete’s foot is characterized by intense itching and burning sensations, particularly between the toes. The discomfort can be persistent and may interfere with daily activities.
iii. Odor and Visible Signs
Dry Skin: Dry skin does not typically produce any odor. The visible signs are limited to the affected area and do not spread to other parts of the body.
Athlete’s Foot: In some cases, athlete’s foot can cause a foul odor due to the fungal infection. The visible signs, such as the rash or blisters, can spread to other areas of the feet and even to the toenails.
iv. Contagiousness
Dry Skin: Dry skin is not contagious. It cannot be spread from person to person or through contact with contaminated surfaces.
Athlete’s Foot: Athlete’s foot is highly contagious. It can spread through direct contact with an infected person or contaminated surfaces, such as shower floors, locker room benches, or shared towels.
The table below summarizes the key differences between dry skin and athlete’s foot:
| Feature | Dry Skin | Athlete’s Foot |
|---|---|---|
| Cause | Environmental factors, medical conditions, aging | Fungal infection (dermatophytes) |
| Appearance | Rough, flaky, scaly skin | Red, scaly rash, peeling or flaking skin, blisters or ulcers |
| Itching | Mild to severe itching | Intense itching and burning sensation |
| Odor | No odor | May have a foul odor |
| Contagiousness | Not contagious | Highly contagious |
Avoiding Missteps: The Significance of Professional Diagnosis
Misdiagnosis can lead to ineffective treatment, prolonged discomfort, and potential complications. Consulting a dermatologist or healthcare provider can ensure an accurate diagnosis and guide you toward the most effective treatment plan for your specific condition.
Misdiagnosis and the Importance of Consulting a Professional
Mistaking dry skin for athlete’s foot, or vice versa, can lead to ineffective treatment, prolonged discomfort, and potential complications.
i. Misdiagnosing dry skin as athlete’s foot:
- Unnecessary antifungal treatment: Using antifungal medications for dry skin is not only ineffective but can also irritate the skin further.
- Delayed treatment for underlying causes: If dry skin is caused by an underlying medical condition, such as eczema or psoriasis, misdiagnosis can delay appropriate treatment, leading to worsening symptoms.
ii. Misdiagnosing Athlete’s Foot as Dry Skin:
- Ineffective treatment: Using moisturizers or lotions for an athlete’s foot will not address the underlying fungal infection, allowing it to persist and spread.
- Increased risk of complications: Untreated athlete’s foot can lead to secondary bacterial infections, which can be more severe and require antibiotic treatment.
iii. When to Seek Professional Consultation
Consult a dermatologist or healthcare provider if you experience any of the following:
- Persistent itching or discomfort on your feet that does not improve with over-the-counter treatments
- Visible signs of infection, such as a red, scaly rash, blisters, or ulcers
- A foul odor emanating from your feet
- Signs of the condition spreading to other areas of your feet or body
- Underlying medical conditions that may affect your skin health, such as diabetes or a weakened immune system
iv. Diagnostic Methods for Differentiating Dry Skin from Athlete’s Foot
Healthcare professionals employ various methods to accurately diagnose the underlying condition:
- Physical examination: A thorough examination of the affected area, including the appearance, texture, and distribution of the skin lesions, can provide valuable clues.
- Medical history review: Understanding your medical history, including any pre-existing skin conditions or risk factors, can aid in the diagnostic process.
- Skin scraping or culture: In some cases, a small skin scraping may be taken and examined under a microscope or cultured to identify the presence of fungal organisms.
Accurate diagnosis is crucial for determining the appropriate treatment plan and ensuring optimal foot
Home Remedies and Self-Care for Dry Skin

Dry skin can be effectively managed with a combination of gentle skincare practices, lifestyle modifications, and over-the-counter products, restoring your feet’s softness and comfort.
i. Hydration and Moisturization: Replenishing Dry Skin
- Bathe or shower with lukewarm water: Avoid hot water, which can strip away natural oils. Limit bathing time to 5-10 minutes.
- Use gentle, fragrance-free cleansers: Harsh soaps can further irritate dry skin. Opt for mild, fragrance-free cleansers designed for sensitive skin.
- Moisturize regularly: Apply a generous amount of moisturizer to your feet, especially after bathing or showering, while the skin is still damp. Choose a moisturizer specifically formulated for dry skin.
ii. Lifestyle Habits to Prevent Dry Skin
- Wear breathable footwear: Avoid tight-fitting or non-breathable shoes that trap moisture and worsen dryness. Opt for natural materials like leather or canvas.
- Protect your feet from harsh elements: Wear socks and shoes in cold weather and avoid prolonged exposure to dry air or extreme temperatures.
- Maintain a healthy diet: A balanced diet rich in essential nutrients, including omega-3 fatty acids and vitamins A, C, and E, can support skin health.
- Hydrate from within: Drink plenty of water throughout the day to keep your skin hydrated from the inside out.
iii. Over-the-counter products for Dry Skin Relief
Emollients:
These products, such as petroleum jelly, help soften and smooth dry skin by filling in the gaps between skin cells.
Our recommendation for Best Emollients on Amazon:
Eucerin Advanced Repair Foot Cream – Fragrance-Free, Foot Lotion for Very Dry Skin
Humectants:
These substances, like hyaluronic acid and glycerin, attract and retain moisture in the skin, providing long-lasting hydration.
Our recommendation for Best Humectants on Amazon:
O’Keeffe’s for Healthy Feet Foot Cream, Guaranteed Relief for Extremely Dry, Cracked Feet
Occlusives:
These products, including shea butter and cocoa butter, create a protective barrier on the skin’s surface, preventing moisture loss.
Our recommendation for Best Occlusives on Amazon:
Treatment Options for Athlete’s Foot
Athlete’s foot requires a multi-pronged approach, encompassing antifungal medications, meticulous hygiene practices, and preventive measures to eradicate the infection and safeguard your foot health.
i. Antifungal Medications:

Antifungal medications are the mainstay of treatment for athlete’s foot. They work by inhibiting the growth and reproduction of the fungal organisms responsible for the infection.
Types of Antifungal Medications:
- Topical antifungals: These creams, lotions, or sprays are applied directly to the affected area. Common topical antifungals include clotrimazole, miconazole, and terbinafine.
- Oral antifungals: In severe or persistent cases, oral antifungal medications may be prescribed. These medications, such as fluconazole and terbinafine, are taken by mouth and work systemically to eliminate the fungus.
ii. Hygiene Practices and Prevention Strategies

In addition to antifungal medications, proper hygiene, and preventive measures are crucial to combat athlete’s foot and prevent recurrence:
- Wash your feet daily with soap and water, paying particular attention to the areas between the toes. Dry your feet thoroughly, especially between the toes, after bathing or showering.
- Wear clean, dry socks made of breathable materials, such as cotton or wool. Change your socks daily, or more often if your feet sweat excessively.
- Choose well-fitting, breathable shoes made of natural materials like leather or canvas. Avoid wearing tight-fitting or non-breathable shoes that trap moisture.
- Avoid sharing towels, footwear, or other personal items with individuals who have athlete’s foot.
- Practice good hygiene in public areas, such as gyms, locker rooms, and swimming pools. Wear shower shoes or sandals in these areas to prevent direct contact with contaminated surfaces.
- Disinfect surfaces regularly, especially in areas where bare feet are common, to minimize the spread of fungal spores.
iii. When to Seek Professional Medical Help
Consult a doctor if:
- Your athlete’s foot symptoms do not improve with over-the-counter antifungal treatments after two weeks.
- The infection is severe, causing extensive blisters, ulcers, or intense discomfort.
- The infection spreads to other areas of your feet, toenails, or other parts of your body.
- You have underlying medical conditions, such as diabetes or a weakened immune system, that may complicate treatment.
Prompt medical attention can ensure a proper diagnosis, custom-made treatment, and effective management of athlete’s foot.
Conclusion
As you navigate the complexities of foot care, the question often arises: Is it dry skin or athlete’s foot? This distinction is critical, as each condition requires a tailored approach to restore foot health.
Dry skin, often caused by environmental factors or underlying medical conditions, responds well to gentle skincare practices, lifestyle modifications, and over-the-counter remedies. In contrast, athlete’s foot, a contagious fungal infection, necessitates antifungal medications, meticulous hygiene practices, and preventive measures to eradicate the infection and prevent recurrence.
Seeking professional guidance is crucial when symptoms persist or intensify. Healthcare providers can accurately diagnose the underlying cause and recommend personalized treatment plans to address your specific needs.
To delve deeper into the intricacies of dry skin and athlete’s foot, including detailed information on prevention, self-care, and professional treatment options, explore the comprehensive guide above.
Share Your Foot Care Journey
Have you encountered dry skin or athlete’s foot? What strategies have you found most effective in managing these conditions? Share your experiences and insights in the comments below, and let’s foster a community of informed and empowered individuals committed to optimal foot health.
FAQ: Is it Dry Skin or Athlete’s Foot
Q: What are the key differences between dry skin and athlete’s foot?
Dry skin is a common condition caused by environmental factors or underlying medical conditions, resulting in flaky, itchy skin. Athlete’s foot is a contagious fungal infection that causes itching, scaling, and blisters, primarily affecting the feet.
Q: How can I prevent dry skin?
Moisturize regularly, use gentle cleansers, wear breathable footwear, and protect your feet from harsh elements.
Q: How can I prevent athlete’s foot?
Keep feet clean and dry, wear shower shoes in public areas, wear breathable socks, alternate shoes, and avoid sharing personal items.
Q: How do I treat dry skin?
Use moisturizers, emollients, humectants, and occlusives. Consult a doctor for severe cases.
Q: How do I treat athlete’s foot?
Use antifungal medications, maintain good hygiene, and practice preventive measures. Seek professional help for persistent or severe cases.
Q: When should I see a doctor?
Consult a doctor if symptoms persist despite self-care, worsen, or spread to other areas.
Q: How can I maintain healthy feet?
Practice regular foot hygiene, wear comfortable shoes, moisturize regularly, and monitor for any changes or concerns.
Sources:
https://www.aad.org/public/diseases/a-z/athletes-foot-prevent
https://www.ncbi.nlm.nih.gov/books/NBK279549/
https://www.cdc.gov/healthywater/hygiene/disease/athletes_foot.html
https://www.webmd.com/skin-problems-and-treatments/understanding-athletes-foot-basics