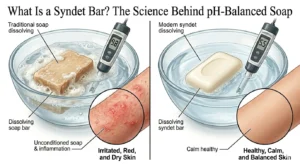
Medicated soap sounds like the responsible choice. It kills bacteria, fights body odour, treats acne, and carries the reassurance of pharmaceutical-grade ingredients. Yet dermatologists consistently advise against using it daily on healthy skin — and the reasons go far deeper than surface-level irritation.
Table of Contents
Toggle- What Is Medicated Soap, Exactly
- The Documented Benefits — When Medicated Soap Genuinely Works
- The Documented Risks — Why Daily Use Is Problematic
- Signs Your Medicated Soap May Be Too Harsh for Your Skin
- Medicated Soap Active Ingredients: Evidence, Uses, and Risks at a Glance
- Common Medicated Soap Brands and What They’re Used For
- When You Should — and Should Not — Use Medicated Soap
- What to Use Instead of Medicated Soap for Daily Cleansing
- Dermatologist-Recommended Cleansers Mentioned in This Guide
- Hibiclens Antimicrobial and Antiseptic Skin Cleanser Liquid
- PanOxyl 10% Benzoyl Peroxide Acne Foaming Wash
- Cetaphil Gentle Cleansing Bar
- Related Cleansers Mentioned in This Guide
- Frequently Asked Questions
- Sources
This guide examines what the evidence actually says about medicated and antibacterial soap: when it genuinely helps, what its documented risks are, which active ingredients to scrutinise, and the exact situations in which a dermatologist would or would not recommend it. What this article does not cover — because it belongs elsewhere — is a deep comparison of all soap types, their pH ranges, and general skin barrier science; for that, see our complete guide to types of soap and their benefits for skin.
⚡ Quick Answer Medicated soap is not bad — when used correctly, for the right condition, for a defined period. Daily use on healthy skin, however, disrupts the skin microbiome, impairs the moisture barrier, and may contribute to antibiotic resistance without providing any proven benefit over plain soap and water.
What Is Medicated Soap, Exactly
Medicated soap contains one or more pharmaceutical-grade active ingredients that perform a therapeutic function beyond basic cleansing. These fall into four main categories based on their target action:
- Antibacterial / antimicrobial: Active agents include chlorhexidine gluconate, benzalkonium chloride, trichlorocarbanilide (TCC), and — until its FDA ban in 2016 — triclosan. These target bacterial pathogens on the skin surface.
- Antifungal: Zinc pyrithione, ketoconazole, and selenium sulphide address fungal infections including tinea versicolor and seborrhoeic dermatitis.
- Anti-acne: Benzoyl peroxide (2.5–10%) and salicylic acid (0.5–2%) are the primary active ingredients in acne-targeted cleansing bars.
- Anti-inflammatory / medicated speciality: Sulphur-based bars (sulphur 3–10%) and coal tar soaps are used for psoriasis and seborrhoeic conditions.
Note on terminology: "Medicated soap" and "antibacterial soap" are often used interchangeably, but they are not identical. All antibacterial soaps are medicated, but medicated soaps also include anti-acne, antifungal, and anti-inflammatory formulations. This distinction matters when evaluating the evidence — the FDA's ruling on triclosan applies specifically to antimicrobial consumer wash products, not all medicated soap categories.
The Documented Benefits — When Medicated Soap Genuinely Works

Peer-reviewed evidence supports medicated and antibacterial soap for several specific conditions. A study published in PMC (National Center for Biotechnology Information) testing 16 medicated soap brands found the majority demonstrated satisfactory antibacterial activity against Staphylococcus aureus, a common skin infection pathogen. [1]
Confirmed Clinical Uses
Hidradenitis suppurativa (HS): Chlorhexidine-based washes are recommended by Cleveland Clinic dermatologist Dr. Michelle Kerns for HS patients because they reduce bacterial load while remaining tolerable for compromised skin. “These products will decrease the bacterial load, but are gentle enough for the skin of people with HS,” Dr. Kerns states. [2]
Surgical site preparation: Chlorhexidine gluconate 4% is the gold standard pre-surgical skin cleanser, reducing post-operative infection rates. This use is outside the scope of consumer soap and under medical supervision.
Acne vulgaris: Benzoyl peroxide cleansing bars reduce Cutibacterium acnes colonisation and free fatty acids in sebum — the primary drivers of acne inflammation. Clinical guidelines from the American Academy of Dermatology list benzoyl peroxide as a first-line acne treatment. [3]
Seborrhoeic dermatitis: Zinc pyrithione and ketoconazole-based medicated bars reduce Malassezia fungal overgrowth, the primary driver of seborrhoeic dermatitis flares on the face, scalp, and body.
Body odour (hyperhidrosis-related): Antibacterial soaps reduce the surface bacteria that convert sweat into odour-producing compounds — a legitimate short-term use in the axillae and groin.
“I can control my HS flare-ups daily with chlorhexidine wash 5%. I apply directly to sores for 10 minutes, then wash off. It dries them up very quickly.” — Verified member, myHSteam patient community (2025). [4]
Clinical context: This outcome is consistent with evidence — chlorhexidine’s effectiveness for HS is well-documented, but it is being used here for a diagnosed condition under guidance, not as a general daily cleanser.
The Documented Risks — Why Daily Use Is Problematic
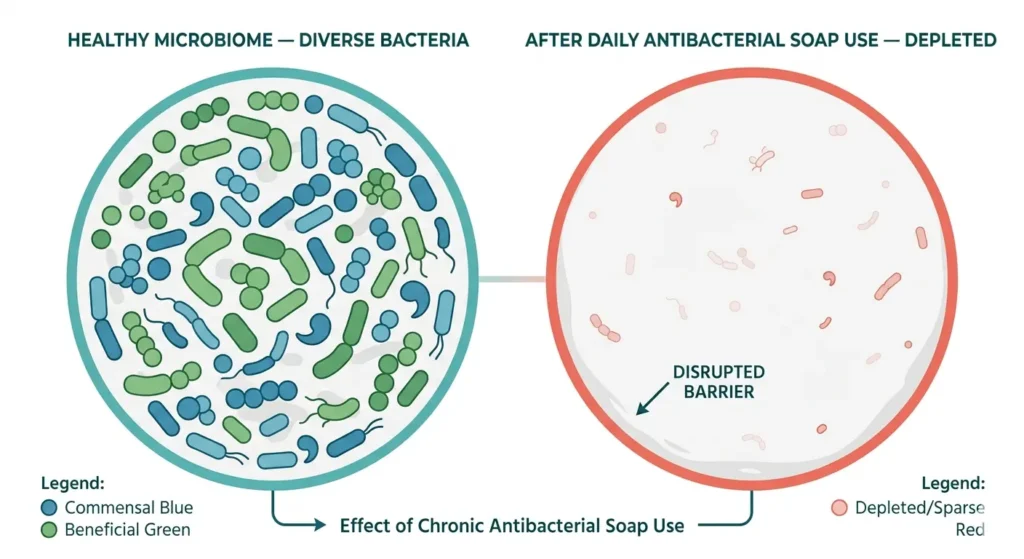
1. Skin Microbiome Disruption
Your skin hosts approximately 1.8 million bacteria per square centimetre — a diverse ecosystem of microorganisms that regulate immune defence, maintain skin pH, and outcompete pathogenic organisms. This is the skin microbiome, and it is not collateral damage to be dismissed when discussing antibacterial soap use.
A peer-reviewed study published in PLOS ONE (Yu et al., 2018, Duke University) found that regular antibacterial soap use significantly altered the skin’s microbial communities, reducing microbial diversity and disrupting microbiome stability. [5]
A 2024 comprehensive review in Heliyon further confirmed that antiseptic skincare products alter normal skin flora — with some changes being actively detrimental to skin health and disease resistance. [6]
In contrast, a 2025 study published in the British Journal of Dermatology found that mild soap bars (specifically a high-glycerine bar) did not negatively affect skin microbiome diversity and actually helped strengthen microbiome network properties. [7]
The implication is clear: the issue is not soap per se — it is the antimicrobial active ingredients in medicated formulations disrupting beneficial bacteria alongside harmful ones.
Why this matters clinically: Depleting the skin microbiome leaves skin vulnerable to opportunistic colonisation by more resistant pathogenic bacteria. Dr. Raina Bembry (Integrated Dermatology of Fairfax) states: “Antibacterial soaps tend to have a higher pH, which can damage the skin barrier. Any damage to the skin barrier can disrupt the skin microbiome by causing an overgrowth or undergrowth of bacteria.” [8]
2. Antimicrobial Resistance
Overexposure to antibacterial agents creates selective pressure — bacteria that survive develop resistance mechanisms, making future infections harder to treat. This concern is not theoretical. The FDA’s 2016 ruling banning 19 active ingredients from consumer antiseptic wash products cited antimicrobial resistance as a primary driver. [9]
The FDA’s formal statement on triclosan — the most widely used antibacterial soap ingredient until its ban — concluded: “Consumers may think antibacterial washes are more effective at preventing the spread of germs, but we have no scientific evidence that they are any better than plain soap and water. In fact, some data suggests that antibacterial ingredients may do more harm than good over the long-term.” — Dr. Janet Woodcock, FDA Center for Drug Evaluation and Research Director. [9]
3. Skin Barrier Damage and Dryness
Most medicated soaps have a pH of 8–11 and contain high-concentration surfactants that strip intercellular lipids from the stratum corneum. For people who already have compromised barrier function — dry skin, eczema, rosacea, or mature skin — this compounds existing damage. Understanding why pH matters so fundamentally is covered in our article on what is a syndet bar and how it protects the skin’s acid mantle.
Dermatologist Dr. Folakemi Cole-Adeife (Lagos State University Teaching Hospital) states unequivocally: “Medicated and antiseptic soaps are recommended by dermatologists only for a controlled, short period of time — not for daily use. Inflammatory conditions like seborrhoeic dermatitis and acne can actually be aggravated by medicated soaps.” [10]
4. Contact Dermatitis and Sensitisation
Several active ingredients in medicated soaps are known contact allergens. Chlorhexidine, despite its clinical effectiveness, causes allergic contact dermatitis in a documented subset of users. Fragrances added to mask the medicinal odour of antiseptic bars are among the top causes of contact dermatitis in adults, according to the American Academy of Dermatology. Repeated exposure to a sensitising ingredient gradually lowers the threshold for reaction — meaning tolerance built over years can disappear, triggering dermatitis from a product used without incident for a long time. For the full list of sensitising soap ingredients, our guide to soap ingredients to avoid for sensitive skin covers each one with clinical evidence.
5. The FDA Triclosan Ban — What It Actually Means for You
In 2016, the FDA issued a final rule removing 19 active antimicrobial ingredients — including triclosan and triclocarban — from consumer antiseptic wash products. The ruling stated that manufacturers had not demonstrated these ingredients were “both safe for long-term daily use and more effective than plain soap and water.” [9]
Animal studies showed potential for hormonal disruption at higher doses, and environmental accumulation concerns were also raised.
Products currently using benzalkonium chloride, benzethonium chloride, or chloroxylenol (PCMX) as triclosan replacements are under ongoing FDA review. These have not been demonstrated unsafe, but the data requirement for long-term daily-use safety has not yet been met.
Practical implication: If your current antibacterial soap uses triclosan — it should no longer be on US shelves. If it lists benzalkonium chloride or PCMX as the active ingredient, it is a post-ban reformulation under ongoing safety review. For healthy skin with no specific condition, these ingredients offer no proven benefit over plain gentle cleanser.
Signs Your Medicated Soap May Be Too Harsh for Your Skin
Many people continue using medicated or antibacterial soap without realizing their skin barrier is already becoming damaged. The problem often starts subtly before progressing into visible irritation.
| Symptom | What It May Mean |
|---|---|
| Tight skin after showering | Barrier oils are being stripped excessively |
| Flaking or rough texture | Skin dehydration and barrier disruption |
| Burning after applying moisturizer | Micro-irritation and increased skin sensitivity |
| Increased oiliness after washing | Compensatory sebum overproduction |
| Itching or redness | Possible irritation or contact dermatitis |
| “Squeaky clean” feeling | Often a sign the skin barrier has been over-stripped |
Important: Healthy skin should feel comfortable after cleansing — not tight, dry, burning, or excessively squeaky-clean. Many people mistakenly interpret that stripped feeling as “extra clean,” when it may actually indicate barrier damage.
Medicated Soap Active Ingredients: Evidence, Uses, and Risks at a Glance
← Scroll left/right on mobile to see full table
| Active Ingredient | What It Targets | Confirmed Benefit | Known Risk with Daily Use | FDA Status |
|---|---|---|---|---|
| Triclosan | Broad-spectrum antibacterial | Hospital-grade infection control | Microbiome disruption, hormone disruption (animal data), antibiotic resistance | Banned in consumer products 2016 |
| Chlorhexidine gluconate | Gram-positive bacteria, surgical prep, HS | Proven for HS, pre-surgical prep | Contact dermatitis, microbiome disruption, barrier damage with overuse | OTC for medical use; not approved as daily consumer soap |
| Benzoyl Peroxide | Cutibacterium acnes (acne) | First-line acne treatment (AAD-endorsed) | Bleaches fabric, skin dryness, irritation at high concentrations | OTC acne drug — approved with restrictions |
| Salicylic Acid | Acne, pore congestion, keratosis | Exfoliates, unclogs pores, anti-acne | Dryness and irritation, not for large body area use | OTC drug — approved |
| Zinc Pyrithione | Malassezia fungal overgrowth | Proven for seborrhoeic dermatitis, dandruff | Generally well-tolerated; occasional irritation | OTC drug — approved |
| Sulphur (3–10%) | Acne, seborrhoeic conditions, psoriasis | Anti-inflammatory, keratolytic | Strong odour, skin dryness, avoid with other actives | OTC drug — approved |
| Benzalkonium Chloride | Broad-spectrum antibacterial | Moderate bactericidal activity | Microbiome disruption, potential sensitisation | Under ongoing FDA review |
Common Medicated Soap Brands and What They’re Used For
Not all medicated soaps use the same active ingredients. Some are designed for acne, while others target bacteria, fungal infections, or body odour. Understanding the active ingredient matters more than the brand name itself.
| Brand | Main Active Ingredient | Common Use | Best For |
|---|---|---|---|
| Dettol | Chloroxylenol (PCMX) | Antibacterial cleansing | Short-term antibacterial use |
| Lifebuoy | Antibacterial agents | General antibacterial cleansing | Body odour and hygiene-focused cleansing |
| Hibiclens | Chlorhexidine gluconate | Medical-grade antimicrobial wash | Pre-surgical cleansing and hidradenitis suppurativa |
| PanOxyl | Benzoyl peroxide | Acne treatment | Body acne and oily skin |
| Cetaphil Gentle Cleansing Bar | Non-medicated syndet formula | Barrier-friendly cleansing | Daily sensitive skin cleansing |
Important: A stronger antibacterial ingredient does not automatically mean a healthier cleanser for daily use. Many dermatologists recommend rotating away from medicated cleansers once the underlying condition improves.
When You Should — and Should Not — Use Medicated Soap
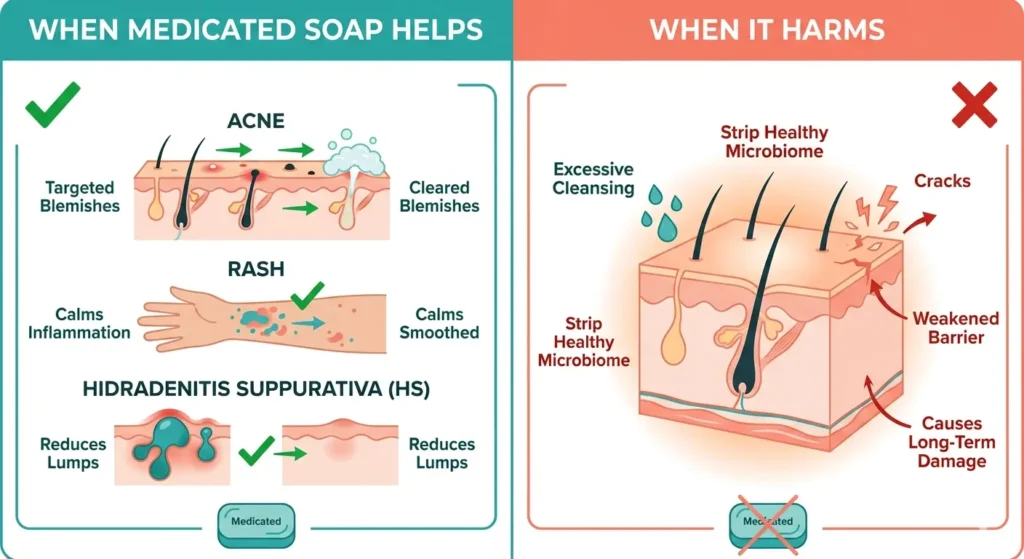
Use Medicated Soap When:
A dermatologist has diagnosed a specific condition that responds to the active ingredient — acne vulgaris, seborrhoeic dermatitis, hidradenitis suppurativa, fungal skin infection, or surgical site preparation. Use it for the prescribed duration (typically 4–12 weeks), then transition to a gentle pH-balanced cleanser. Target the affected area — do not apply a medicated acne bar to your entire body if only your face is affected.
Do Not Use Medicated Soap When:
Your skin is healthy and you are using it for perceived hygiene benefit. The FDA has confirmed no evidence that antibacterial soap is superior to plain soap and water for infection prevention in healthy individuals. Do not use it if you have dry skin, eczema, rosacea, or a compromised barrier — the antimicrobial agents will worsen barrier integrity and microbiome balance. Do not use it on children without paediatric dermatologist guidance — children’s skin barrier is still developing and significantly more vulnerable to disruption.
The “better safe than clean” myth: Using medicated soap daily is not a hygiene upgrade — it is a net negative for most people’s skin health. For healthy skin, a gentle pH-balanced syndet bar or glycerin bar cleans as effectively as any antimicrobial formulation, without the documented microbiome and barrier trade-offs.
The Transition Protocol — Switching Off Medicated Soap
If you have been using medicated soap daily and want to switch, do not switch cold. A sudden change can temporarily destabilise the skin barrier as microbiome communities re-establish. Dermatologists recommend: reduce medicated soap to every other day for two weeks → then switch to a fragrance-free syndet or glycerin bar for daily use → apply a ceramide-based moisturiser after each wash to support barrier recovery. Expect a 2–4 week adjustment period before skin settles.
What to Use Instead of Medicated Soap for Daily Cleansing
For most skin types and conditions, a syndet bar (pH 5.5–7.0) or a glycerin-based cleanser delivers effective cleansing without antimicrobial agents that the FDA has confirmed are unnecessary for general hygiene. For dry or sensitive skin, our guide to the best soap for dry skin covers the clinical evidence behind each gentler alternative in full.
For acne specifically: if you are using medicated soap with benzoyl peroxide or salicylic acid, continue under dermatologist guidance. Once acne is controlled, transitioning to a non-medicated salicylic acid toner (leave-on product) while using a gentle cleanser often provides better long-term outcomes — because it reduces the stripping effect on the skin barrier that daily medicated cleansers cause.
Dermatologist-Recommended Cleansers Mentioned in This Guide
If you’re trying to move away from harsh daily antibacterial soaps, these are some of the most commonly recommended cleanser types discussed throughout this article.
Related Cleansers Mentioned in This Guide
These options match the cleanser types discussed above. Choose based on your skin concern — not because a product sounds stronger or more “medical.”
Hibiclens Antimicrobial and Antiseptic Skin Cleanser Liquid
Best for short-term antiseptic cleansing and targeted hygiene use when suitable for your skin concern.
Who can use it: Adults needing temporary antiseptic cleansing.
Key ingredient type: Isopropyl Alcohol 4% w/v.
Use carefully if: your skin is dry, irritated, sensitive, or eczema-prone.
PanOxyl 10% Benzoyl Peroxide Acne Foaming Wash
Best for body acne, oily skin, back acne, chest acne, and acne-prone areas.
Who can use it: People with acne-prone or oily skin who tolerate benzoyl peroxide.
Key ingredient type: Benzoyl peroxide acne cleanser.
Use carefully if: skin becomes dry, tight, peeling, or irritated.
Cetaphil Gentle Cleansing Bar
Best for daily cleansing, dry skin, sensitive skin, and switching away from harsh antibacterial soaps.
Who can use it: Most people with normal, dry, or sensitive skin.
Key ingredient type: Non-medicated gentle cleansing bar.
Use carefully if: you are allergic to any listed ingredient.
Disclosure: Some links may be affiliate links. Product ingredients can change, so always check the label before use. This section is educational and does not replace dermatologist advice.
Frequently Asked Questions
Is antibacterial soap better than regular soap?
No — the FDA has formally confirmed that antibacterial soap is not more effective than plain soap and water for the general public. For healthy individuals, a 20-second wash with any gentle cleanser is sufficient for infection prevention. Antibacterial soaps carry additional documented risks including microbiome disruption and potential antimicrobial resistance. [9]
Can medicated soap cause skin dryness?
Yes — most medicated soap formulations have a high pH (8–11) and contain concentrated surfactants that strip intercellular lipids from the stratum corneum, elevating transepidermal water loss (TEWL). This is particularly damaging for people with already-dry or compromised skin. If you experience dryness, tightness, or flaking after using a medicated soap, this is a clear signal to switch to a gentler, pH-balanced alternative. The ingredients most likely causing dryness are the antimicrobial actives combined with SLS as a surfactant.
Can I use medicated soap every day for acne?
Benzoyl peroxide and salicylic acid face wash bars can be used daily as part of an acne treatment regimen, but dermatologists typically recommend them for a defined treatment period rather than indefinitely. Over time, daily medicated cleansing can over-dry the skin, triggering compensatory sebum overproduction that worsens acne. If your skin feels tight or dry after using an acne wash, reduce frequency to every other day or switch to a leave-on benzoyl peroxide product with a gentler cleanser.
Is triclosan still in soap products?
Triclosan was banned from consumer antiseptic wash products in the US in 2016. [9] It may still appear in non-wash products (some toothpastes, medical devices) and in products sold in countries without equivalent regulations. If you are buying soap outside the US or EU, check the ingredient list for triclosan (CAS 3380-34-5) or its synonyms (5-chloro-2-(2,4-dichlorophenoxy)phenol).
What soap should I use after stopping medicated soap?
Transition to a fragrance-free syndet bar or glycerin-based cleanser at pH 5.5–7.0. These cleanse effectively without antimicrobial agents, preserve the acid mantle, and support microbiome recovery. If you were using medicated soap for acne, a non-medicated salicylic acid toner as a leave-on product — combined with a gentle cleanser — often produces better long-term outcomes. For dry or sensitive skin, our guide to the best soap for dry skin provides specific evidence-backed options.
Can I use Dettol soap every day?
Daily use of antibacterial soaps like Dettol may over-dry healthy skin and disrupt the skin microbiome over time. While these soaps can help reduce bacteria temporarily, dermatologists generally recommend using them only when medically necessary — such as during fungal infections, body odour issues, or specific skin conditions. For daily cleansing, a gentle pH-balanced cleanser is usually safer for long-term skin health.
What happens if you use antibacterial soap every day?
Overusing antibacterial soap daily may damage the skin barrier, reduce healthy skin bacteria, and increase dryness, irritation, tightness, and sensitivity. Some antibacterial ingredients may also contribute to antimicrobial resistance over time. According to the FDA, antibacterial soap has not been proven more effective than plain soap and water for healthy individuals.
Can medicated soap darken skin?
Medicated soap itself does not directly darken skin, but excessive dryness and irritation from overuse may trigger post-inflammatory hyperpigmentation in sensitive individuals. This is more common in darker skin tones after repeated irritation or barrier damage.
Is medicated soap good for pimples?
Some medicated soaps containing benzoyl peroxide or salicylic acid can help mild acne and pimples by reducing excess oil and acne-causing bacteria. However, overusing harsh acne soaps may worsen irritation and dryness. Dermatologists usually recommend balancing acne treatment with a gentle cleanser and moisturizer.
Can children use medicated soap?
Children’s skin barriers are thinner and more sensitive than adult skin. Unless recommended by a pediatrician or dermatologist for a diagnosed condition, medicated soaps are generally not advised for daily use in children.
How often should you use medicated soap?
Medicated soap should usually be used only for a specific condition and for a limited period recommended by a dermatologist. For most people, daily long-term use is unnecessary and may damage the skin barrier.
Summary — What You Need to Know
- Medicated soap is clinically effective for specific diagnosed conditions: acne, HS, seborrhoeic dermatitis, fungal infections, and surgical site preparation. It is not a daily hygiene upgrade.
- Daily use on healthy skin disrupts the skin microbiome, impairs the moisture barrier, and may contribute to antimicrobial resistance — with no proven benefit over plain soap and water (FDA, 2016).
- The FDA banned triclosan and 18 other antibacterial ingredients from consumer soaps in 2016. Replacement ingredients (benzalkonium chloride, PCMX) are under ongoing safety review.
- If prescribed medicated soap for a condition, use it targeted to the affected area for the defined treatment period, then transition to a gentle pH-balanced cleanser.
- For daily cleansing on healthy skin: a syndet bar or glycerin-based cleanser at pH 5.5–7.0 is the evidence-supported alternative — effective, safe, and microbiome-friendly.
Sources
All claims in this article are sourced from peer-reviewed research, FDA regulatory communications, and verified dermatologist expert commentary.
- Antimicrobial Activity of Medicated Soaps, PMC3224419. ncbi.nlm.nih.gov
- Dr. Michelle Kerns, Cleveland Clinic. Best Soap for Hidradenitis Suppurativa (2025). clevelandclinic.org
- American Academy of Dermatology. Acne Treatment: Medications. aad.org
- myHSteam. Best Soaps for Hidradenitis Suppurativa (2025). myhsteam.com
- Yu J et al. (2018). Antibacterial soap use impacts skin microbial communities. PLOS ONE. PMC6101359. ncbi.nlm.nih.gov
- Dong Z et al. (2024). Skin care products and the skin microbiome. Heliyon. PMC11298934. ncbi.nlm.nih.gov
- Mild skin cleansers strengthen microbiome networks (2025). British Journal of Dermatology. PubMed 41118317. pubmed.ncbi.nlm.nih.gov
- Dr. Raina Bembry. Integrated Dermatology of Fairfax. Antibacterial Soap and the Skin Microbiome. fairfaxderm.com
- FDA. Skip the Antibacterial Soap; Use Plain Soap and Water. fda.gov
- Dr. Folakemi Cole-Adeife. PUNCH HealthWise interview (2023). healthwise.punchng.com
Medical Disclaimer: This article is for educational purposes only and does not constitute medical advice. If you have a diagnosed skin condition, consult a board-certified dermatologist before changing your cleanser or stopping a prescribed medicated soap regimen.
📚 Continue the Soap Science Series